
Understanding Why It Happens — and the Pathway to Surgical Reconstruction For many women, a hysterectomy brings relief from difficult symptoms such as heavy bleeding, fibroids, or chronic pelvic pain. After recovery, life often returns to normal. However, months or even years later, some women begin to experience new and unexpected symptoms — a feeling […]
Understanding Why It Happens — and the Pathway to Surgical Reconstruction
For many women, a hysterectomy brings relief from difficult symptoms such as heavy bleeding, fibroids, or chronic pelvic pain. After recovery, life often returns to normal.
However, months or even years later, some women begin to experience new and unexpected symptoms — a feeling of heaviness in the pelvis, discomfort when standing for long periods, or the sensation that something is “falling down.”
These symptoms can be confusing and sometimes distressing, especially when they appear long after the original surgery. In many cases, they may be caused by a condition known as vaginal vault prolapse, a form of pelvic support failure that can occur after a hysterectomy.
Understanding why this happens — and how it can be effectively treated — is the first step toward restoring comfort and quality of life.
What Is Vaginal Vault Prolapse?
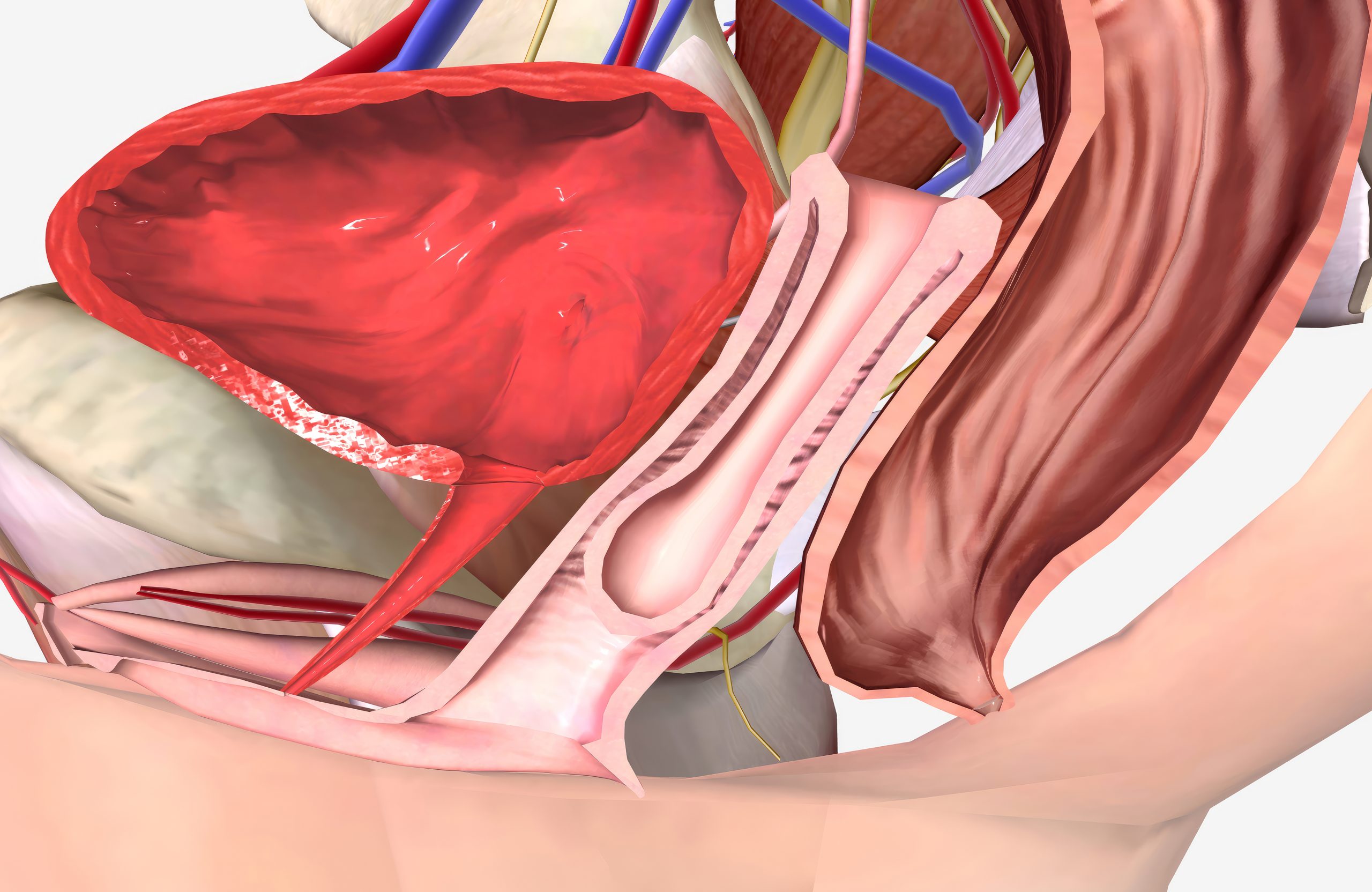
During a hysterectomy, the uterus is surgically removed. After the uterus is removed, the top portion of the vagina — known as the vaginal vault — remains and is supported by surrounding tissues and ligaments within the pelvis.
In most cases these support structures continue to function well. However, over time, the tissues responsible for holding the vaginal vault in its normal position can weaken. When this support is no longer strong enough, the top of the vagina may begin to descend downward into the vaginal canal.
This condition is known as vaginal vault prolapse.
One of the most challenging aspects of this condition is that it does not always occur immediately after surgery. Many women develop symptoms years after their hysterectomy, which can make the connection between the two events difficult to recognise.
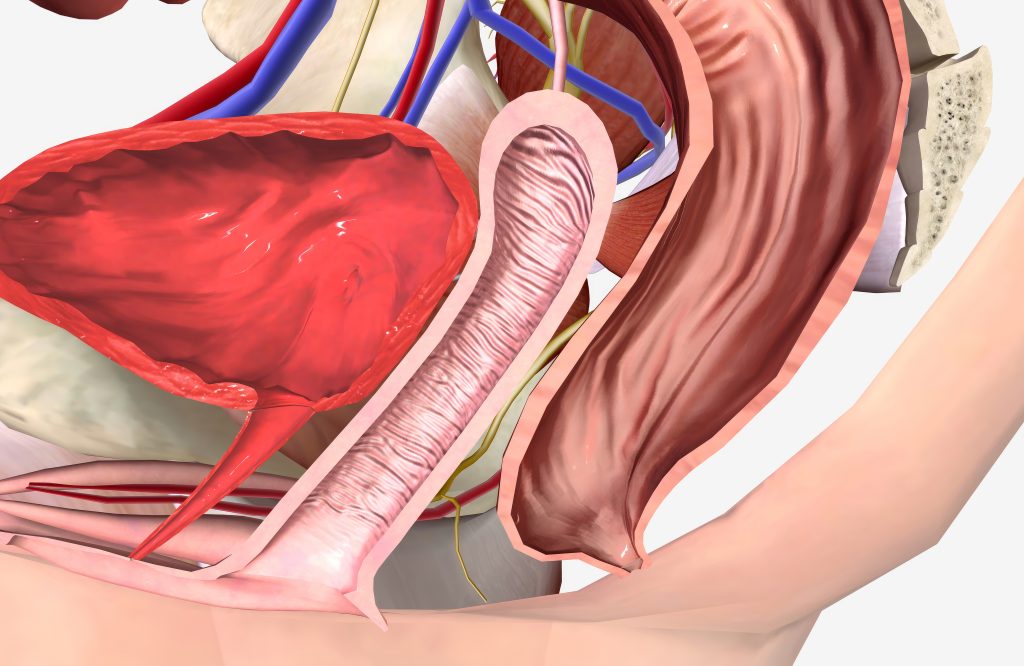
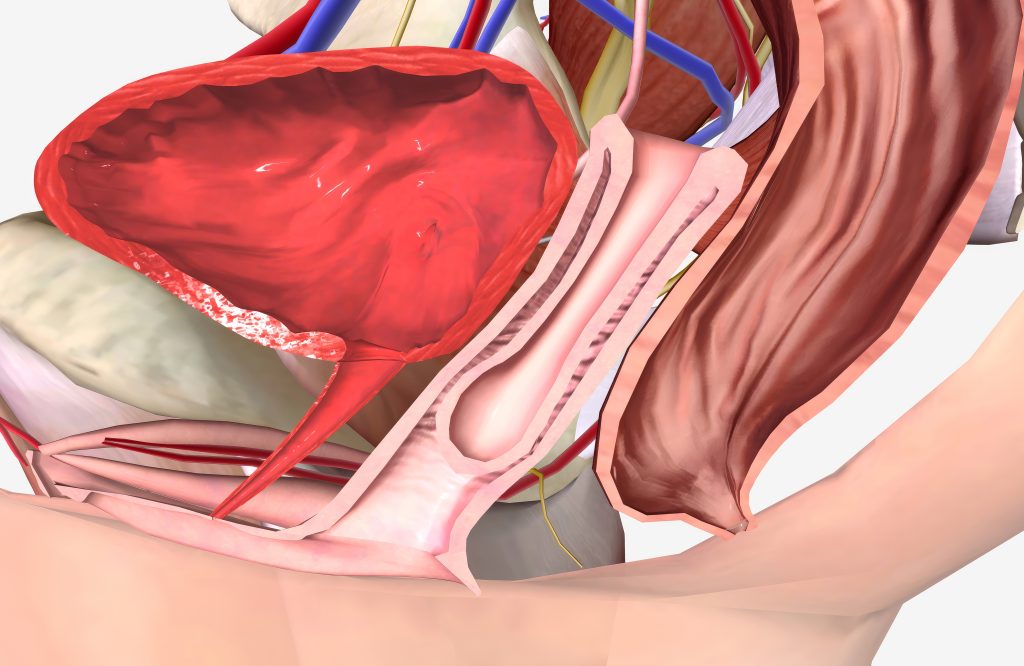
Why Can Prolapse Develop After a Hysterectomy?
A hysterectomy changes the structural dynamics of the pelvis. The uterus normally plays an important role in the pelvic support system, and its removal alters how surrounding tissues carry and distribute pressure within the abdomen.
Over time, several factors can contribute to the weakening of pelvic support structures. These may include the natural ageing process of connective tissues, the long-term effects of childbirth, and everyday increases in abdominal pressure caused by activities such as lifting, coughing, or straining.
It is important to note that hysterectomy itself does not automatically lead to prolapse. Many women never develop this complication. However, because the pelvic support system has changed, some women may become more susceptible to structural weakening over time.
When this happens, the vaginal vault may gradually lose its support and begin to descend.
Recognising the Signs
The symptoms of vaginal vault prolapse can vary, but many women describe a similar experience.
One of the most common signs is a sensation of heaviness or pressure in the pelvis, particularly toward the end of the day or after prolonged standing. Some women notice a bulging sensation in the vagina or feel as though something is descending internally.
Other symptoms may include discomfort during physical activity, difficulty emptying the bladder fully, or changes in sexual comfort.
Because these symptoms often develop gradually, many women delay seeking help, assuming that the changes are simply part of ageing or something they must live with. In reality, vaginal vault prolapse is a treatable structural condition, and effective surgical solutions are available.
When Surgical Reconstruction Becomes the Right Solution
Vaginal vault prolapse is fundamentally a support problem. The tissues that normally hold the vaginal vault in its correct position have weakened, allowing it to descend.
For this reason, treatment focuses on restoring strong and durable support to the vaginal vault. The goal of surgical reconstruction is to reposition the vaginal vault and secure it in a stable anatomical position so that normal pelvic function can be restored.
Successful surgery can relieve the sensation of pressure, improve bladder function, and allow women to return comfortably to daily activities.
Reconstructive Surgery for Vaginal Vault Prolapse
One of the most effective surgical procedures used to correct vaginal vault prolapse is called sacrocolpopexy.
During this procedure, the vaginal vault is carefully repositioned and supported by attaching it to a strong ligament along the sacrum, which is part of the lower spine. This creates durable support for the top of the vagina and restores its normal anatomical position.
Today, this surgery is frequently performed using minimally invasive laparoscopic or robotic-assisted techniques. For patients, this typically means less postoperative discomfort, shorter hospital stays, and faster recovery times, while still achieving strong and lasting structural repair.
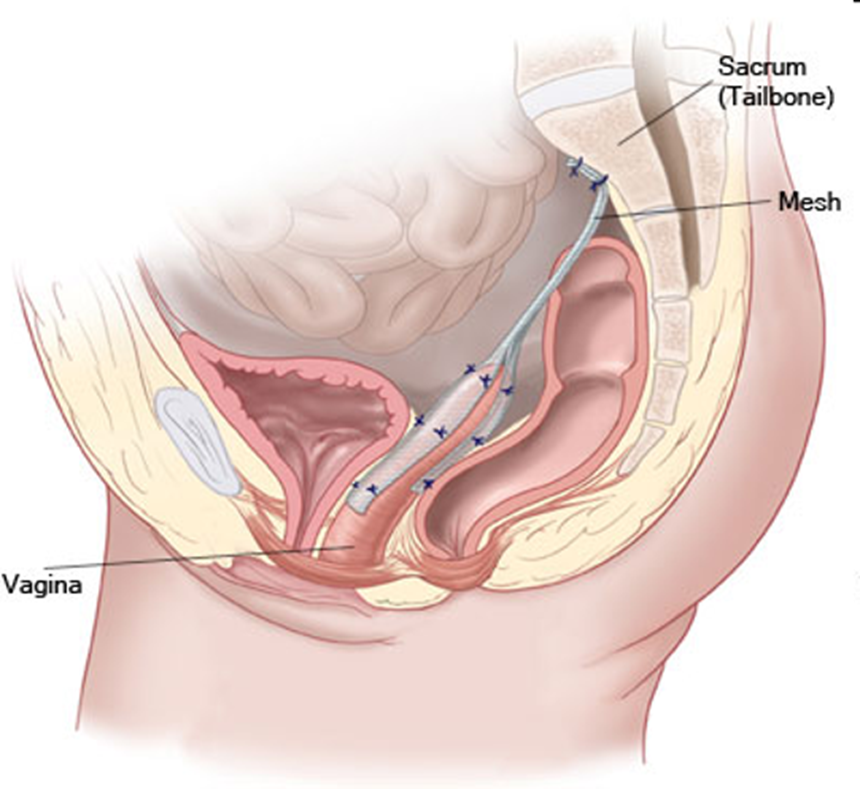
In the past, some vaginal prolapse repairs were performed using mesh placed through a vaginal approach. However, concerns about complications associated with transvaginal mesh led to significant international scrutiny. As a result, the use of transvaginal mesh for prolapse repair has been widely discontinued and banned in many countries, and international professional bodies, including the International Urogyneacological Association (IUGA), no longer support this approach for routine prolapse surgery.
Today, when mesh is used for prolapse reconstruction, it is typically placed laparoscopically from the abdominal side, during procedures such as sacrocolpopexy. In this approach, the mesh is positioned to support the vaginal vault by attaching it to the sacrum, allowing the prolapse to be corrected while restoring strong anatomical support.
This minimally invasive abdominal technique has become the preferred surgical method for vaginal vault prolapse repair, as it provides durable support while avoiding the complications historically associated with transvaginal mesh placement.
Why Specialist Surgical Expertise Matters
Surgery for vaginal vault prolapse can become technically complex, particularly in patients who have had previous pelvic surgery or whose anatomy has changed significantly since their hysterectomy.
In these situations, reconstructing pelvic support requires a detailed understanding of pelvic anatomy and extensive experience with advanced minimally invasive surgical techniques.
Because of this, many patients are referred to surgeons who specialise in pelvic reconstructive surgery, particularly when the condition requires complex laparoscopic or robotic-assisted procedures.
Specialist expertise plays an important role in ensuring that the vaginal vault is restored securely and that the long-term results of surgery are durable.
Dr MC Conradie’s Role in Pelvic Reconstructive Surgery
Dr MC Conradie specialises in minimally invasive urological and pelvic reconstructive surgery, including advanced laparoscopic and robotic procedures used to restore pelvic support.
Her practice focuses on complex surgical conditions of the urogenital system, and she frequently manages patients who require specialised reconstructive procedures following previous pelvic surgery.
Through minimally invasive techniques, Dr Conradie performs procedures designed to restore anatomical support while minimising surgical trauma and supporting a smoother recovery for patients.
For women experiencing vaginal vault prolapse after hysterectomy, evaluation by a surgeon experienced in advanced reconstructive techniques can play an important role in achieving successful and lasting outcomes.
Restoring Comfort and Quality of Life
Experiencing symptoms of prolapse after a hysterectomy can be unsettling, especially when the connection between the original surgery and new symptoms is not immediately clear.
The encouraging reality is that vaginal vault prolapse is a condition that can be effectively treated. Modern reconstructive surgery offers the ability to restore pelvic support, relieve symptoms, and allow women to return to daily life with renewed comfort and confidence.
No one should feel that they must simply live with the symptoms of pelvic support failure. With the right expertise and surgical approach, lasting solutions are available.
If you are experiencing symptoms following a hysterectomy, consultation with a specialist experienced in advanced pelvic reconstructive surgery may help determine the most appropriate treatment pathway. For more information or to arrange a consultation, contact Dr MC Conradie Inc..