For many patients, the idea of removing a kidney can seem surprisingly straightforward. Because humans are born with two kidneys, it is often assumed that losing one is unlikely to have significant long-term consequences. Patients are frequently reassured that they can live a normal life with a single kidney, and in many cases this is […]
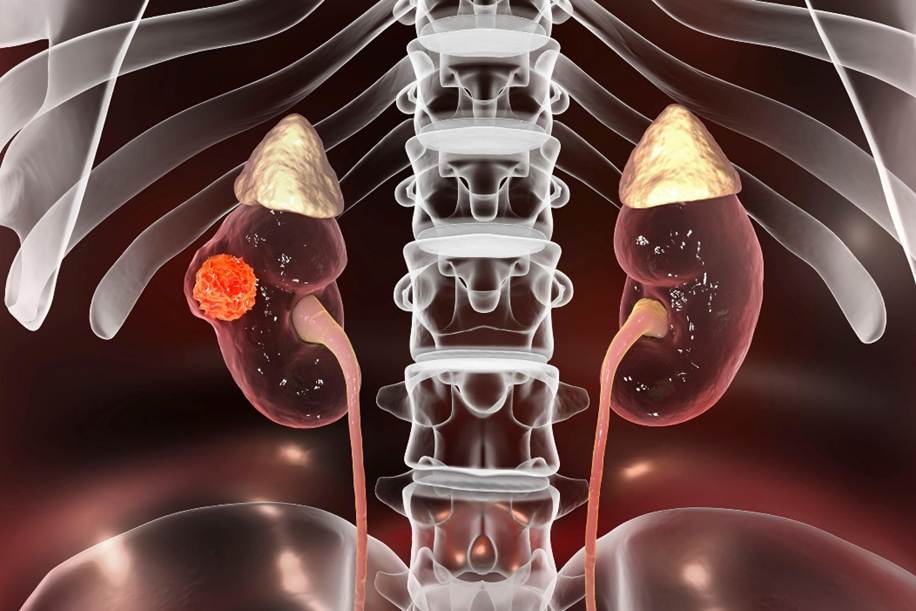
For many patients, the idea of removing a kidney can seem surprisingly straightforward. Because humans are born with two kidneys, it is often assumed that losing one is unlikely to have significant long-term consequences. Patients are frequently reassured that they can live a normal life with a single kidney, and in many cases this is true.
However, the question that deserves closer consideration is not simply whether a person can live with one kidney — but whether removing it was truly necessary in the first place.
Modern urology has increasingly shifted toward a different perspective: whenever possible, preserving kidney function should be a priority. This shift reflects a deeper understanding of how important the kidneys are to long-term health and why removing one can have consequences that extend far beyond the immediate surgical problem.

The Role of the Kidneys in Long-Term Health
The kidneys are among the body’s most important organs. They are responsible for filtering waste products from the blood, maintaining the balance of fluids and electrolytes, regulating blood pressure, and producing hormones that influence red blood cell production and metabolic stability.
Although the body can adapt when one kidney is removed, the two kidneys function as part of a carefully balanced physiological system. Each contributes to maintaining the body’s internal environment with remarkable precision.
When one kidney is removed, the remaining kidney typically compensates by increasing its workload. Over time, it may enlarge and take on a greater share of filtration. This adaptive process allows many people to continue living healthy lives. However, adaptation is not the same as preservation.
Reducing the body’s total kidney reserve can have important implications for a patient’s health over the long term.
What Happens After a Kidney Is Removed
Following nephrectomy — the surgical removal of a kidney — the body undergoes several adjustments. The remaining kidney increases its filtration capacity to compensate for the loss of the other. In the short term, this process is often effective, and patients may feel no immediate difference in their daily lives.
But over time, the long-term implications of having reduced kidney reserve may become more significant.
Studies have shown that patients living with a single kidney may face increased risks in certain circumstances, including:
For many patients, these risks remain relatively small and manageable. Nevertheless, they highlight an important principle in modern urological care: preserving kidney function whenever possible helps protect a patient’s long-term health.
This is why the decision to remove a kidney must always be considered carefully.
The Difference Between Removing and Preserving
In urological surgery, treating kidney disease often involves choosing between two fundamentally different approaches.
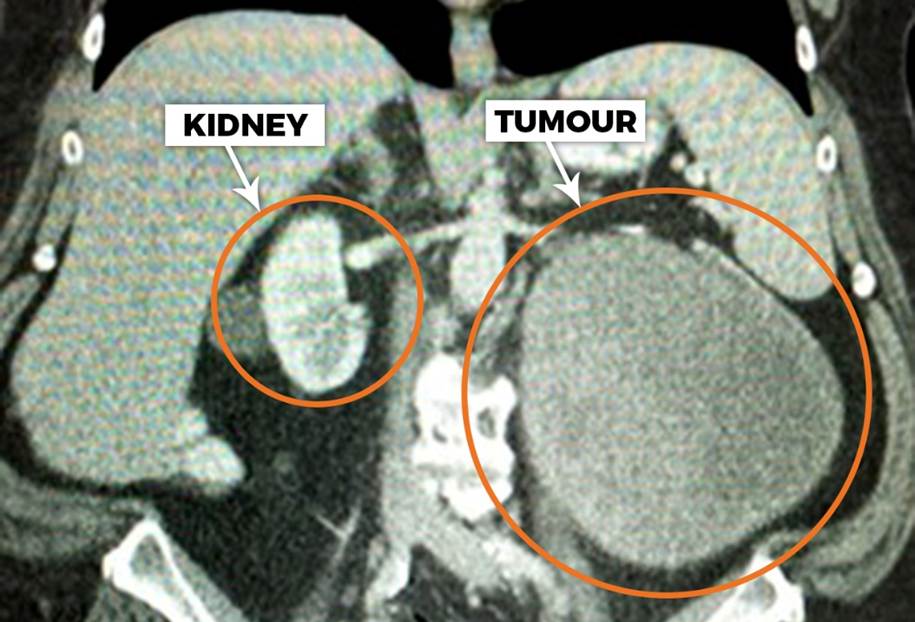
The first approach is radical nephrectomy, where the entire kidney is removed along with the disease. This procedure is technically reliable and, in many cases, appropriate. When a kidney is severely damaged or affected by large or aggressive tumours, removal may be the safest option.
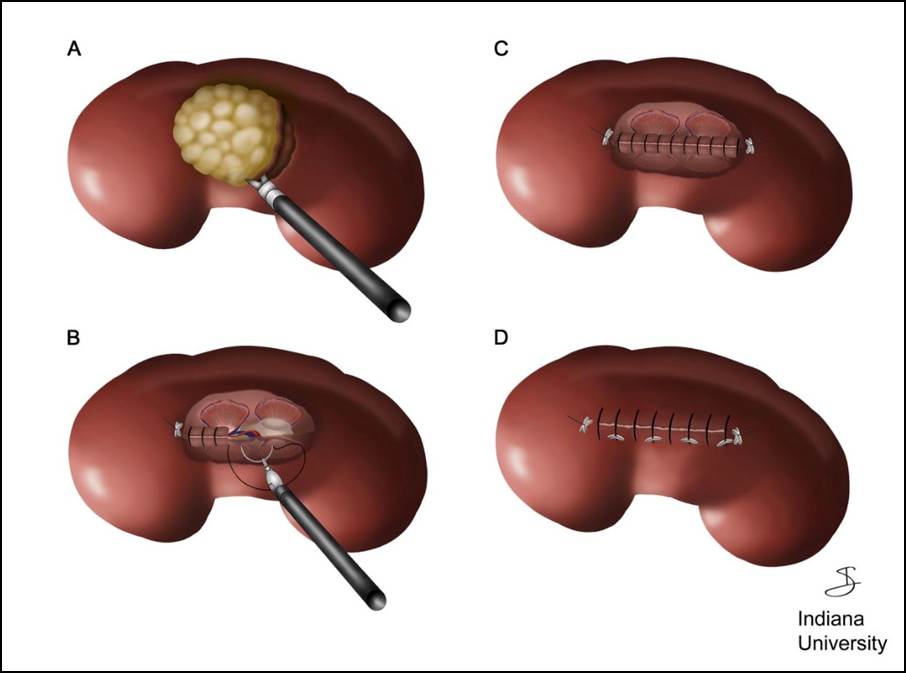
The second approach is kidney-preserving surgery, most commonly in the form of partial nephrectomy or reconstructive procedures. In these operations, the surgeon removes the diseased portion of the kidney while preserving as much healthy tissue as possible.
While both approaches can be effective, the difference between them is significant.
Removing a kidney often involves fewer reconstruction steps and a more straightforward surgical pathway. Preserving a kidney, however, requires a much higher level of technical precision. Surgeons must carefully remove the problem while maintaining blood supply, protecting surrounding structures, and reconstructing the remaining kidney tissue so that it continues to function normally.
Organ preservation is therefore not simply a different procedure. It represents a more complex surgical challenge.
How Minimally Invasive Surgery Has Changed What Is Possible
Over the past two decades, advances in minimally invasive surgery have dramatically expanded the ability of surgeons to preserve organs while treating disease.
Laparoscopic and robotic techniques now allow surgeons to operate with extraordinary precision inside delicate anatomical spaces. These techniques provide enhanced visual magnification, improved instrument control, and access to areas that were once extremely difficult to treat without large open operations.
In modern urology, these advances have made it possible to:
Importantly, these techniques are not simply about smaller incisions. They represent a fundamental shift in how surgery is performed — moving from removing organs to restoring normal anatomy and function whenever possible.
However, the success of these procedures depends heavily on surgical experience and careful planning.
Dr MC Conradie’s Approach: Protecting the Patient’s Future
With extensive experience in advanced laparoscopic kidney surgery and reconstructive procedures, her approach focuses on preserving kidney function whenever it is safely possible.
Over the course of her career, she has performed thousands of laparoscopic kidney operations, including complex tumour resections and reconstructive procedures designed to maintain normal urinary function.
Each case begins with careful evaluation and detailed surgical planning. The objective is not simply to remove disease, but to correct the underlying problem while protecting the patient’s long-term health.
Whenever feasible, kidney-preserving strategies are considered first. By combining minimally invasive techniques with advanced reconstructive skill, it is often possible to treat complex conditions while maintaining healthy kidney tissue.
This approach reflects a broader responsibility in modern surgery: not only solving the immediate medical problem, but protecting the patient’s future wellbeing.
When Kidney Removal Is Still Necessary
Despite the advances in surgical techniques, there remain situations where removing a kidney is the most responsible course of action.
This may be the case when:
In these circumstances, nephrectomy remains an important and often life-saving procedure.
Responsible surgical care means recognising when preservation is possible — and when it is not.
The Question Patients Should Be Asking
When patients are told that kidney surgery may be necessary, the conversation often focuses on whether surgery can be avoided. But a more important question may be:
Can the kidney be preserved?
This question shifts the focus toward long-term health rather than simply addressing the immediate condition. In many cases, advances in modern urology mean that problems that once required organ removal can now be treated while preserving kidney function.
Understanding the full range of options requires evaluation by a surgeon experienced in advanced minimally invasive and reconstructive techniques.
Taking the Next Step
If you have been advised that a kidney may need to be removed, or if you are seeking a second opinion regarding your treatment options, specialist evaluation may help determine whether kidney-preserving surgery is possible.
For referring physicians, complex renal tumours and structural kidney conditions may benefit from assessment by a surgeon experienced in advanced laparoscopic and reconstructive urology.
Dr MC Conradie provides expert evaluation and treatment for complex urological conditions, with a strong focus on minimally invasive techniques and organ preservation whenever possible. To schedule a consultation with Dr Conradie or to refer a patient for specialist assessment, contact the practice to arrange an appointment and explore the most appropriate path forward.