
Minimally invasive surgery is often described in simple terms. Smaller incisions. Less pain. Faster recovery. While these benefits are real, they only tell part of the story. What patients don’t see is the level of skill required behind those smaller incisions. Because in reality, minimally invasive surgery is not a simpler version of traditional surgery. […]
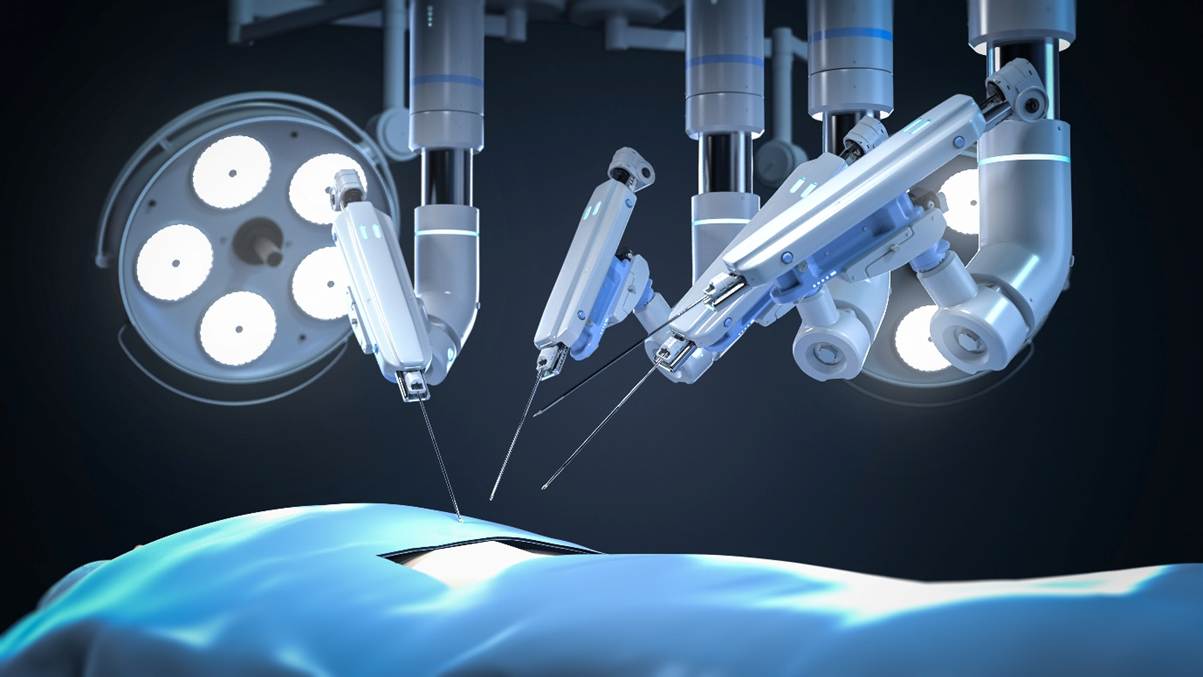
Minimally invasive surgery is often described in simple terms.
Smaller incisions. Less pain. Faster recovery.
While these benefits are real, they only tell part of the story. What patients don’t see is the level of skill required behind those smaller incisions. Because in reality, minimally invasive surgery is not a simpler version of traditional surgery. In many ways, it is significantly more complex.
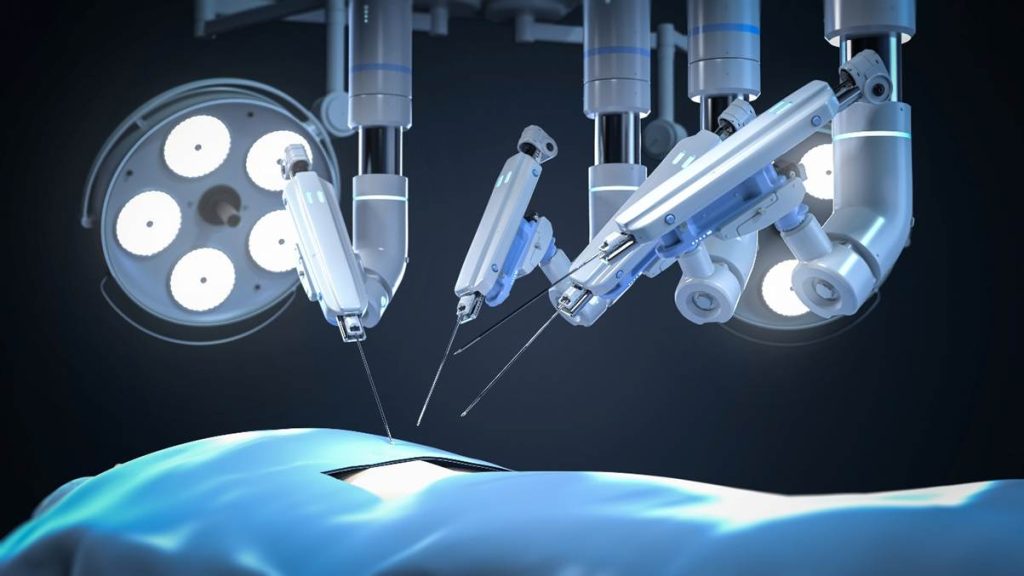
What Minimally Invasive Surgery Really Involves
In traditional open surgery, the surgeon operates with direct access to the affected area — using their hands, with full visibility and tactile feedback. Minimally invasive surgery changes that entirely.
Procedures are performed through small ports using a camera and specialised instruments. The surgeon operates while viewing a magnified image on a screen, guiding long instruments within a confined space, without direct contact with the tissue.
Every movement is controlled externally, while the work is performed internally. This requires a different way of operating — one that depends heavily on visual precision, spatial awareness, and controlled movement.
What appears minimal on the outside demands a high level of precision on the inside.
Laparoscopic surgery introduces a number of technical challenges that are not present in open procedures:
These factors mean that every movement must be deliberate, accurate, and controlled.
There is very little margin for error.
The Learning Curve
Mastering minimally invasive surgery takes time — and volume. Unlike many other surgical techniques, laparoscopic procedures have a steep and prolonged learning curve. Developing proficiency requires not only formal training, but repeated exposure to a wide range of cases.
Surgeons must learn to:
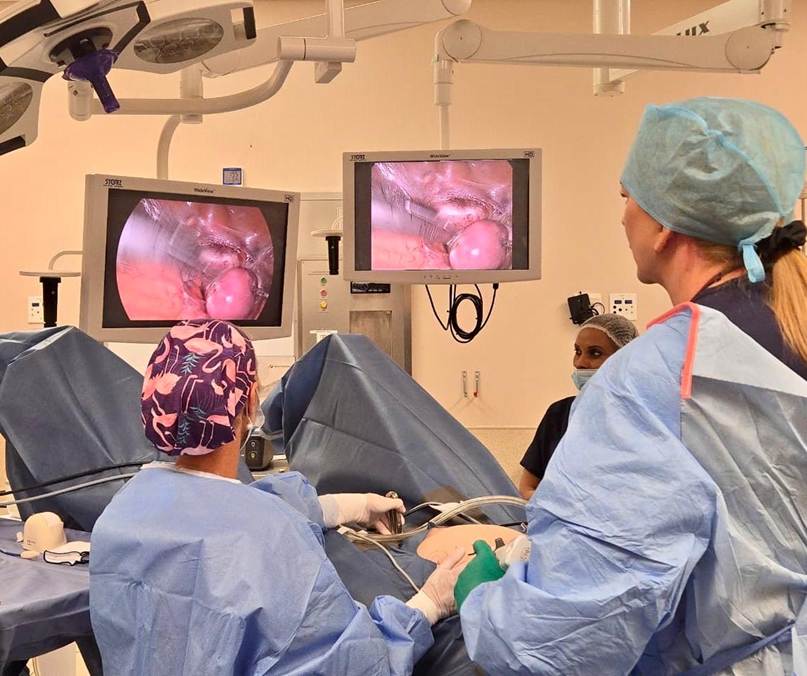
This level of skill is not developed quickly. It is built gradually, through years of practice and refinement.
Why Experience Matters
In minimally invasive surgery, experience directly influences outcomes.
It affects:
While the techniques themselves are widely known, the ability to apply them consistently — particularly in complex cases — depends on depth of experience. Minimally invasive surgery is not defined only by the tools used. It is defined by the expertise of the surgeon using them.
Experience in Practice
Dr MC Conradie’s work in minimally invasive urology reflects this level of expertise. With more than 5,000 laparoscopic kidney procedures performed — including radical nephrectomy, partial nephrectomy, and advanced reconstructive surgeries — her experience spans both routine and highly complex cases.
This volume of work provides more than technical familiarity. It builds the ability to:
In complex urological surgery, this depth of experience becomes critical — not only in performing the operation, but in ensuring the best possible outcome for the patient.
The Skill Patients Don’t See
For patients, the most visible outcome of minimally invasive surgery is often the smallest detail — the size of the incision. What remains unseen is the process behind it.
This is the quiet skill behind minimally invasive surgery. It is not defined by what is visible after the procedure — but by the level of expertise required to perform it effectively.
Minimally invasive surgery is not about doing less. It is about doing more — with greater precision, less disruption, and a stronger focus on preserving normal function. As surgical techniques continue to evolve, so too does the level of skill required to perform them well.
For patients, this highlights an important consideration:
Not all minimally invasive surgery is the same.
The outcome depends not only on the technique, but on the experience and expertise of the surgeon performing it.
Taking the Next Step
If you are considering urological surgery or have been advised to explore minimally invasive options, it is important to understand what the procedure involves — and who will be performing it.
For patients, this means seeking care from a specialist with significant experience in advanced laparoscopic techniques. For referring physicians, complex urological cases may benefit from evaluation by a surgeon with extensive exposure to minimally invasive and reconstructive procedures.
Dr MC Conradie provides expert assessment and surgical care in advanced urology, with a strong focus on precision, experience, and patient outcomes.
To schedule a consultation or refer a patient, contact the practice to arrange an appointment.